CEREBROFLOW
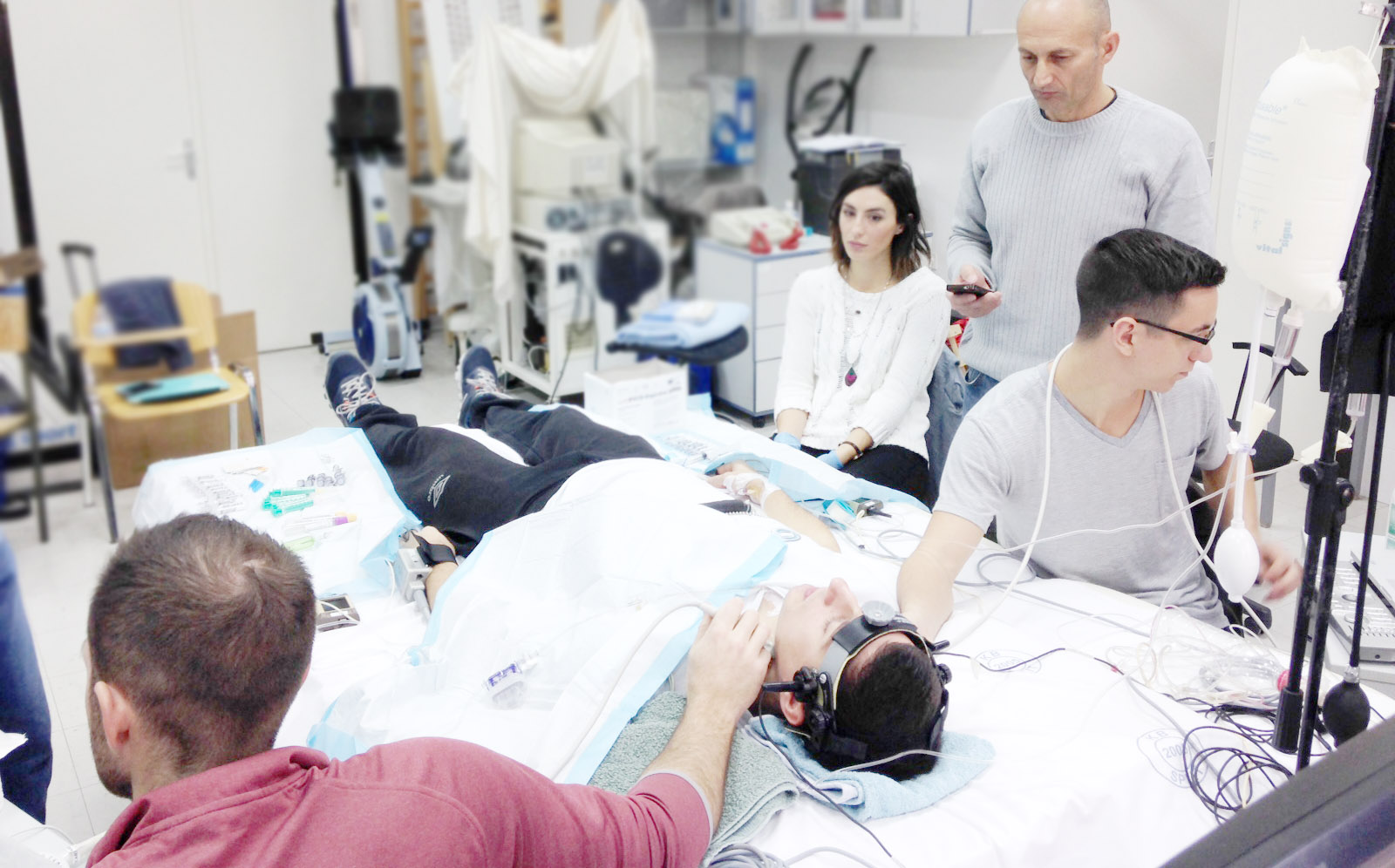
Project title: „Cerebrovascular regulation during apnea in elite breath-hold divers“
Project duration: 28.9.2015. – 28.9.2019.
Funding agency: Croatian Science Foundation
Project leader:
Željko Dujić, Full professor, University of Split School of medicine, Croatia
Researchers:
Phillip Ainslie, Full professor, University of British Columbia, Canada
Kevin Shoemaker, Full professor, School of Kinesiology, Western University, Canada
Otto Barak, Postdoctoral researcher, Faculty of Medicine, University of Novi Sad, Serbia
Tonći Batinić, Assistant professor, Clinical Hospital Center Split, Croatia
Mihajlo Lojpur, Assistant professor, Clinical Hospital Center Split, Croatia
Marijana Karlović-Vidaković, PhD student, Clinical Hospital Mostar, Bosnia
Krešimir Čaljkušić, PhD student, Clinical Hospital Center Split, Croatia
Ivan Drviš, Assistant professor, University of Zagreb, Faculty of Kinesiology, Croatia
Damir Fabijanić, Associate professor, Clinical Hospital Center Split, Croatia
Toni Brešković, Research associate, University of Split School of medicine, Croatia
Arne Sieber, Associate professor, Chalmers University of Technology, Gothenburg, Sweden
Tanja Mijačika, PhD student, University of Split School of medicine, Croatia
Project summary:
The main objective of this proposal is to propose and conduct a series of incrementally progressive studies to examine new physiological questions in apnea diving physiology, with particular focus on brain physiology and the related integration with circulatory and respiratory reflexes. Addressing the novel questions outlined in this proposal will enrich our understanding of the fundamental mechanisms governing cerebral blood flow in conditions of severe hypoxia. Characterization of these relationships between oxygen, cerebral perfusion and cerebral metabolism, and their respective importance on brain homeostasis is a fundamental step toward raising our understanding of brain physiology to that of other body systems. Breath holding exerts a potent stress to the cardiovascular system and brain, yet elite breath-hold divers are able to tolerate marked reductions in blood oxygenation that only sometimes results in loss of consciousness (syncope). The mechanisms allowing such tolerance to hypoxemic extremes may serve as a useful model for the study of cerebrovascular regulation during physiological duress often observed in trauma and disease. This is especially true given that the study of regional brain perfusion during cardiorespiratory challenges, exercise, and in pathology has only begun in the past several years. Thus, the study of regional cerebrovascular regulation and its relation to the circulatory and ventilatory in healthy, trained breath-hold divers will yield new insight into the cerebrovascular function and systems integration in humans. Moreover, elucidation of these mechanistic relationships is paramount to our comprehension of myriad pathologies associated with arterial hypoxemia and/or elevations in blood viscosity or hemoglobin levels.
Specific aims:
#1: to examine the effects of indomethacin on CBF reduction and maximal breath-hold time.
#2: to quantify the role of peripheral chemosensation on hemodynamics and breath-hold time in elite BHD.
#3: to quantify the hemodynamic responses during a maximal breath-hold with and without beta-blockade administration.
#4: to quantify CMRO
2 and cerebral substrate utilization during a prolonged breath-hold that yields severe levels of hypoxemia and hypercapnia, and to partition the influence of breathing versus apnea at similar arterial blood gases on CMRO
2 and substrate usage.
#5: to determine the magnitude of the NO, oxygen free radical and FMD responses in trained BHD after a single and repetitive maximal breath hold in dry or immersed conditions.
#6: to determine the CBV response to simulated breath hold in elite divers, and to separate the effects of hypoxia and hypercapnic hypoxia on CBV.
#7: to determine the pulmonary vascular pressure response during prolonged apnea in trained breath hold divers, to examine whether changes in right heart pressure impact on left ventricular function and to examine myocardial mechanics during breath hold to investigate the underlying cardiac physiology during significant hemodynamic changes.
#8: to determine the impact of chemoreflex, baroreflex, lung stretch receptors and 'drive-to-breathe' in voluntary apnea.
#9: to determine if both the MCA and PCA constricts during hypocapnia and/or dilates during hypercapnia and to quantify the impact of such change on CBF.
#10: to determine the extent to which the intra-cranial blood vessels constrict during different levels of hyperoxia and/or dilate during different levels of hypoxia and to quantify the impact of such change son CBF.
#11: to examine the reactivity of the cerebral arteries to a maximal breath-hold.
#12: to measure CBF, CMRO
2 and carbohydrates during pre-breathing pure oxygen and during following maximal breath hold while immersed in the shallow laboratory pool.
#13: to measure vital physiological parameters during pool or open sea dives in different apnea disciplines such as static and dynamic apnea and no limit.


 Ispiši stranicu
Ispiši stranicu


